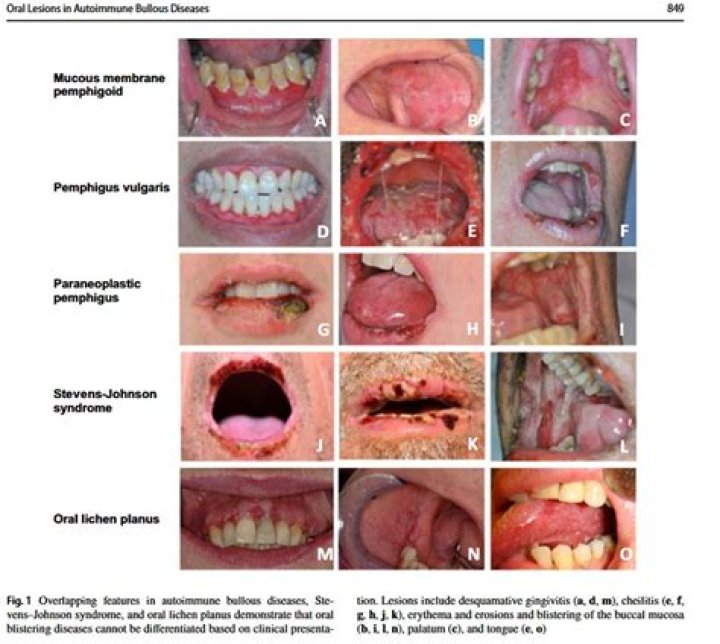
A condition in which the edge of the gums near the teeth become red and inflamed. Linear gingival erythema is common with HIV infection.
How is linear gingival erythema treated?
The etiopathogenesis of linear gingival erythema is uncertain, although some investigators hypothesize that the condition results from subgingival colonization and tissue invasion by Candida species. Treatment may include débridement, povidone-iodine irrigation, chlorhexidine mouth rinse, and/or antifungal therapy.
What is the meaning of gingival inflammation?
Overview. Gingivitis is a common and mild form of gum disease (periodontal disease) that causes irritation, redness and swelling (inflammation) of your gingiva, the part of your gum around the base of your teeth.
What is the cause of linear gingival erythema?
Linear gingival erythema is a condition that’s related to a fungal infection of the gums. It appears as a red line along the gum line and causes pain and sometimes bleeding. This condition is one of the most common oral complications of HIV. However, people with HIV aren’t the only ones can who develop LGE.What are the stages of gingivitis?
- Gingivitis. …
- Periodontitis – Stage 1: Initial. …
- Periodontitis – Stage 2: Moderate. …
- Periodontitis – Stage 3: Severe (with potential for tooth loss) …
- Periodontitis – Stage 4: Severe (with potential for the loss of all teeth)
What does red band gingivitis look like?
LGE is a form of gingivitis characterized by a distinct red band (2-3 mm in width) along the gingival margin. In some cases it presents as small petechial-like patches on the gingiva. It presents most frequently in anterior teeth but it can extend to the posterior teeth, in some case bleeding and discomfort occur.
What bacteria causes acute necrotizing ulcerative gingivitis?
Acute Necrotizing Ulcerative Gingivitis (ANUG), more commonly known as “trench mouth” for its common occurrence among soldiers in the trenches during World War I, is a painful gum disease caused by the gram negative bacteria known as spirochetes.
What is plasma cell gingivitis?
Plasma cell gingivitis [PCG] is a rare benign condition of the gingiva characterized by sharply demarcated erythematous and edematous gingivitis often extending to the mucogingival junction. As the name suggests it is diffuse and massive infiltration of plasma cells into the sub-epithelial gingival tissue.What is hereditary gingival fibromatosis?
Hereditary gingival fibromatosis (HGF) is a rare disorder characterized by a benign, non-hemorrhagic, fibrous gingival overgrowth that can appear in isolation or as part of a syndrome. Clinically, a pink gingiva with marked stippling can be seen to cover almost all the tooth, in many cases preventing eruption.
What is marginal gingivitis?Accumulations of dental plaque adjacent to the gingival margin which result in gingival inflammation have been termed marginal gingivitis. Recently an international consensus report defined gingival disease. The two broad categories were plaque-induced disease and non-plaque-induced disease.
Article first time published onIs my gingivitis healing?
In most cases, gingivitis usually clears up within 10 to 14 days. If your gingivitis is more serious, it could take longer to treat. Take charge of your dental health to prevent it from recurring.
How can I get rid of gingivitis fast?
- Brush Your Teeth Twice a Day. Use a soft-bristled toothbrush to gently brush around each tooth. …
- Floss Your Teeth Once a Day. Plaque loves to hide in between teeth where toothbrush bristles can’t reach. …
- Use a Fluoride Mouth Rinse. …
- Don’t Skip Dental Appointments. …
- Avoid Sugary Foods and Beverages.
How long does gingivitis take to heal?
Treatment Time for Gingivitis But for those with gingivitis due to poor oral hygiene, the average time it takes for gingivitis to go away is about 10 to 14 days after your treatment, along with proper oral healthcare. Keep in mind that there are many, many factors that can change the timeline.
Do your gums grow back after gingivitis?
The simple answer is, no. If your gums are damaged by, for example periodontitis, the most severe form of gum disease, it’s not possible for receding gums to grow back. However, even though receding gums can’t be reversed there are treatments that can help to stop the problem from getting worse.
What is Stage 3 gum disease?
Stage 3: Moderate Periodontitis Infections in the area can create bleeding, pus development, and pain around the teeth. Gum recession can make the teeth sensitive and uncomfortable. As the gums pull away from the teeth, the teeth lose their natural support system and they can become loose.
Do antibiotics help gingivitis?
Gum disease like periodontitis or gingivitis can be treated with antibiotics, although they are not recommended as the sole treatment.
What does gum necrosis look like?
Features seen on examination: Ulceration and necrosis of the gum margin between the teeth, initially with loss of the tip of gum usually seen between two teeth. It is mainly the gum margin that is affected resulting in loss of gum architecture. White pseudomembrane may be seen over the necrotic area(s).
What antibiotics treat necrotizing ulcerative gingivitis?
Treatment. For any signs of systemic involvement, the recommended antibiotics are: Amoxicillin, 250 mg 3 x daily for 7 days and/or. Metronidazole, 250 mg 3 x daily for 7 days.
Which disease is associated with necrotizing ulcerative periodontitis?
Necrotizing periodontitis is a rapidly destructive subcategory within necrotizing periodontal diseases. The most commonly noted predisposing factor of necrotizing ulcerative periodontitis (NUP) is an immunocompromised state, such as that found in patients with HIV.
What does periodontal disease smell like?
It is the smell of deep infection and rot. For patient’s with this condition, they may even be unaware that they have this problem. And if they are aware, they may try to cover up the condition with gum or breath mints or toothbrushing.
What toothpaste is best for gingivitis?
- Best Overall (Anti-Cavity) —Crest Pro-Health Advanced Deep Clean.
- Best Toothpaste for Gingivitis —Parodontax Toothpaste for Gingivitis.
How do you know if gingivitis is getting worse?
- Red, Swollen Gums that Bleed Easily. …
- Loose or Shifting Teeth. …
- Chronic Bad Breath. …
- Gum Recession. …
- Pus between the Teeth. …
- Developing Health Conditions.
How is gingival fibromatosis treated?
Gingival fibromatosis is removed by gingivectomy, recurrences are treated in the same fashion or by more conservative removal of local areas of hyperplasia. Improved oral hygiene and topical antibiotics will greatly diminish the risk of recurrence. DIGH may also be treated by gingivectomy and plaque control.
What causes gingival fibromatosis?
Gingival fibromatosis can be caused by number of factors including inflammation, leukemic infiltration, and use of medications such as phenytoin, cyclosporine or nifedipine,[14] and vigabatrin. [19] Gingival enlargement can be part of Laband, Rutherford, Ramon, or Cross syndrome.
How is gingival fibromatosis diagnosed?
Diagnosis is made based on medical history, clinical examination, blood tests and histopathological evaluation of affected gingival tissue. Differential diagnosis includes consideration of all pathologies in the mouth that involve excessive accumulation of gingival tissue, including syndromic HGF.
How is plasma cell gingivitis treated?
Non surgical therapy included thorough oral prophylaxis, oral hygiene instructions and an antihistamine mouthwash. The patient was instructed to avoid possible allergens like chewing gums, cosmetics and food additives. A strict elimination diet was advised and a change of the regular toothpaste was tried.
What causes plasma cell gingivitis?
Causes. Plasma cell gingivitis and plasma cell cheilitis are thought to be hypersensitivity reactions to some antigen. Possible sources of antigens include ingredients in toothpastes, chewing gum, mints, pepper, or foods. Specifically, cinnamonaldehyde and cinnamon flavoring are often to blame.
What produce plasma cells?
Plasma cells, also called plasma B cells, are white blood cells that originate in the lymphoid organs as B lymphocytes and secrete large quantities of proteins called antibodies in response to being presented specific substances called antigens. …
Is gingivitis serious?
Gingivitis means inflammation of the gums, or gingiva. It commonly occurs because a film of plaque, or bacteria, accumulates on the teeth. Gingivitis is a non-destructive type of periodontal disease, but untreated gingivitis can progress to periodontitis. This is more serious and can eventually lead to loss of teeth.
What is the most common type of gingivitis?
Gingivitis has been classified by clinical appearance (eg, ulcerative, hemorrhagic, necrotizing, purulent), etiology (eg, drug-induced, hormonal, nutritional, infectious, plaque-induced), and duration (acute, chronic). The most common type of gingivitis is a chronic form induced by plaque.
Where is gingival margin located?
The free gingival margin is the area located in between the sulcular epithelium and the epithelium of the oral cavity. This interface exists at the most coronal point of the gingiva. This is also referred to as the crest of the marginal gingiva.