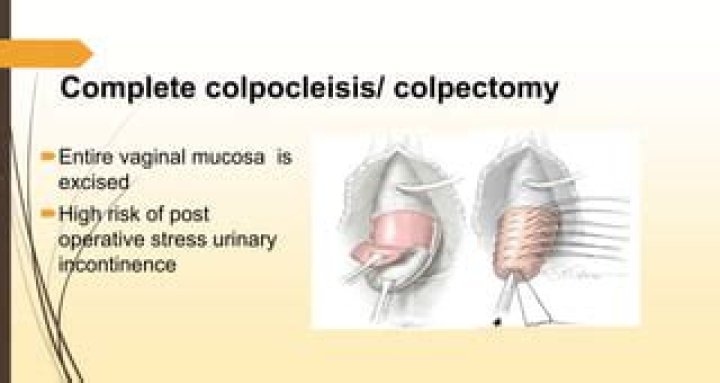
A colpectomy is the surgical removal of all or part of the vagina. It is a minimally invasive and very successful way to treat pelvic organ prolapse in women that are no longer sexually active.
What is the meaning of Colpectomy?
A colpectomy is the surgical removal of all or part of the vagina. It is a minimally invasive and very successful way to treat pelvic organ prolapse in women that are no longer sexually active.
What is the purpose of a Colpoplasty?
Colpoplasty, which is defined as plastic surgery involving the vagina, has the ability to change the way the urinary tract functions for women.
Can I get my vagina sewn up?
This procedure may also be done if an older woman’s vagina severely sags or drops into the vaginal canal (vaginal vault prolapse). In this surgery, the vagina is sewn shut. So it is only done if the woman no longer desires sexual intercourse.Is vaginal obliteration reversible?
No. Because the vagina will be closed permanently, this surgery is only usually recommended for older women who are no longer engaged in sexual activity, or for those who don’t foresee having intercourse in the future.
How do you treat BUWA?
- Perform Kegel exercises to strengthen pelvic muscles and support the weakened fascia.
- Avoid constipation by eating high-fiber foods and drinking plenty of fluids.
- Avoid bearing down to move your bowels.
- Avoid heavy lifting.
- Control coughing.
- Lose weight if you’re overweight or obese.
What is the CPT code for Colpectomy?
Subjects were identified by their Current Procedural Terminology (CPT) codes and categorized into 3 groups: (1) partial or complete vagi- nectomy/colpectomy (CPT 57106, 57110); (2) vaginal hysterectomy with total or partial colpectomy (CPT 58275, 58280); and (3) Le Fort colpocleisis (CPT 57120).
What does Colpoplasty mean in medical terms?
: surgical repair of the vaginal wall.Why is a Colpopexy performed?
Sacral colpopexy, also known as sacrocolpopexy or sacrospinous colpopexy, is a surgical procedure used to correct pelvic organ prolapse in women. When the muscles around a woman’s pelvis weaken, the pelvic organs can prolapse (slide out of place).
How do you perform a Culdocentesis?During a culdocentesis a long thin needle is inserted through the vaginal wall just below the uterus and a sample is taken of the fluid within the abdominal cavity. Culdocentesis is a procedure which checks for abnormal fluid in the space that is just behind the vagina, the posterior cul-de-sac.
Article first time published onHow do you fix a prolapse without surgery?
The two non-surgical options for prolapse are pelvic floor muscle training (PFMT) and a vaginal pessary. PFMT can be effective for mild prolapse but is usually not successful for moderate and advanced prolapse. The main alternative to surgery for prolapse is a vaginal pessary.
Do you have to wear a pessary forever?
Will I have to wear a pessary forever? Pessaries are a safe, long-term management option for pelvic organ prolapse. Some women happily use pessaries for years. Other women choose to just wear their pessary for exercise and physical activity.
Can you bill a cystoscopy with a hysterectomy?
It is strongly recommended to perform cystoscopy at the conclusion of any hysterectomy done for an indication that includes uterovaginal prolapse. The cystoscopy must assess for and document at a minimum the integrity of the bladder as well as patency of the ureters.
What is a rectocele repair?
The goal of rectocele repair is to strengthen the wall between the vagina and rectum. In this surgical procedure, the doctor will make an incision into the back wall of the vagina. The layers under the vaginal wall are then sutured together in such a way as to tighten the tissues and reinforce the strength of the wall.
How do you bill for bladder instillation?
A: Billing should include CPT code 51720 Bladder instillation of anticarcinogenic agent (including retention time) for the instillation procedure and J9030 BCG live intravesical, 1 mg in line 24D of the CMS 1500 Claim form, and 25 Units in line 24G of the CMS 1500 Claim form.
Why am I throbbing down there?
This happens because there is increased blood flow to the area and the muscles of the vaginal wall may have some minor contractions. The vagina also has arteries that supply blood to the area, and it is possible in some women to feel their pulse in certain spots.
Is Sacrocolpopexy a major surgery?
Sacrocolpopexy is a major surgical procedure to treat prolapse of the vault (top) of the vagina in women who have had a previous hysterectomy by fixing it to the sacrum using a graft or mesh.
How long does Sacrocolpopexy surgery take?
The surgery takes 2-3 hours to complete. When it is over, the patient will be taken to the Post-Anesthesia Care Unit (PACU) to wake up from anesthesia.
What happens after anterior and posterior repair?
After an Anterior and Posterior Vaginal surgery Usually both the pack and catheter are removed within 24 – 48 hours after the operation. Once the catheter has been removed it is normal to monitor how much your bladder holds and whether or not you completely empty your bladder when you go to the toilet.
What does Hyster o mean?
What does hystero- mean? Hystero- is a combining form used like a prefix representing the word uterus, also known as the womb, where offspring are conceived and gestate in mammals. It is often used in medical terms, especially in anatomy. … The combining form metro- can also indicate uterus.
What does CEPT mean in drugs?
A combining form for a drug formed when a receptor is fused to the Fc portion of an immunoglobulin G molecule.
What is a McCall Culdoplasty?
The modified McCall Culdoplasty procedure is a relatively simple procedure that is performed after removal of the uterus and cervix from the apex of the vagina wherein the angles of the vagina are attached to their respective uterosacral ligament and the cul-de-sac is surgically obliterated for support postoperatively.
What is Culdocentesis used for?
Culdocentesis may be used to evaluate women with pain in the lower abdomen/pelvis to determine whether intraabdominal fluid is present and, if present, to reveal the nature of the fluid (eg, serous, purulent, bloody).
Why does blood from Culdocentesis not clot?
Blood from a patient’s peri- toneal cavity does not clot very easily due to the fact that there are certain proteins in the peritoneal cavity that prevent this. However, clots are still possible especially when a woman has an old rup- tured ectopic.
What is positive Culdocentesis?
A positive tap is one in which more than 2 mL of nonclotting blood is obtained. Absolute volume may be related to the needle position or the rate of bleeding, so larger amounts of blood have no particular significance. Approximately 82-95% of ectopic pregnancies display nonclotting blood on culdocentesis.
What happens if prolapse is left untreated?
If prolapse is left untreated, over time it may stay the same or slowly get worse. In rare cases, severe prolapse can cause obstruction of the kidneys or urinary retention (inability to pass urine). This may lead to kidney damage or infection.
Can prolapse fix itself?
Prolapsed organs cannot heal themselves, and most worsen over time.
What is a Stage 3 prolapse?
Degrees of uterine prolapse Stage I – the uterus is in the upper half of the vagina. Stage II – the uterus has descended nearly to the opening of the vagina. Stage III – the uterus protrudes out of the vagina. Stage IV – the uterus is completely out of the vagina.
Is a pessary better than surgery?
Although POP surgery has several advantages over pessary treatment, the risk of complications is higher and it might be less cost-effective. Since previous studies have shown promising results with pessary treatment, it might be an equivalent option in the treatment of POP, probably with less risk and lower cost.
Does walking help pelvic floor?
Exercising weak muscles regularly, over a period of time can strengthen them and make them work effectively again. Regular gentle exercise, such as walking can also help to strengthen your pelvic floor muscles.
Is walking good for bladder prolapse?
walking – this is the best exercise during bladder prolapse surgery recovery. doing pelvic floor exercises. resting each day.