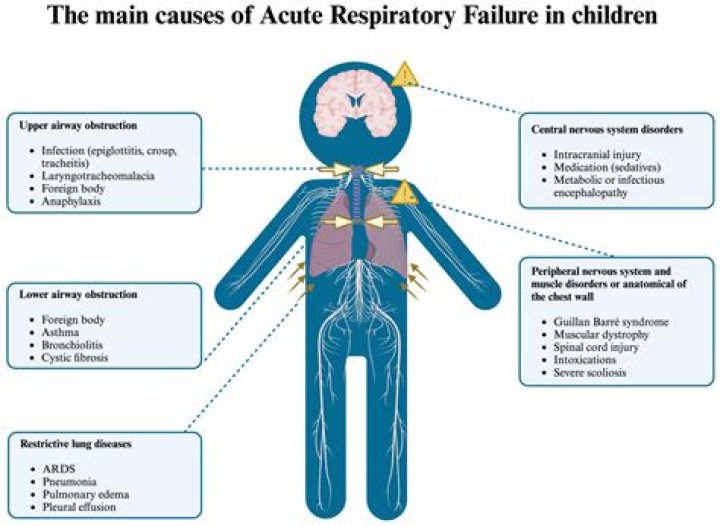
When a person has acute respiratory failure, the usual exchange between oxygen and carbon dioxide in the lungs does not occur. As a result, enough oxygen cannot reach the heart, brain, or the rest of the body. This can cause symptoms such as shortness of breath, a bluish tint in the face and lips, and confusion.
How do you assess for acute respiratory failure?
Assessment of respiratory sounds may include inspiratory or expiratory ‘wheeze‘, which may indicate bronchospasm. Upper airway secretions may also be heard as gurgling sounds. Chest movement should be assessed for its symmetry and pattern.
What two parameters are most important when determining respiratory failure?
Two BLS vital sign measurements that are helpful in assessing and monitoring the degree of respiratory distress are respiratory rate and oxygen saturation.
What are the associated clinical indicators of ARDS?
- Severe shortness of breath.
- Labored and unusually rapid breathing.
- Low blood pressure.
- Confusion and extreme tiredness.
What is a full respiratory assessment?
The ability to carry out and document a full respiratory assessment is an essential skill for all nurses. The elements included are: an initial assessment, history taking, inspection, palpation, percussion, auscultation and further investigations.
What is clinically significant acute respiratory distress?
Acute respiratory distress syndrome is a manifestation of acute injury to the lung, commonly resulting from sepsis, trauma, and severe pulmonary infections. Clinically, it is characterized by dyspnea, profound hypoxemia, decreased lung compliance, and diffuse bilateral infiltrates on chest radiography.
What are the signs of acute respiratory infection?
- Chest or nasal congestion.
- Wet or dry cough.
- Runny nose.
- Fatigue.
- Body aches.
- Low-grade fever.
- Sore throat.
What ABG results would indicate acute respiratory failure?
Using the P/F Ratio to Identify Acute Respiratory Failure The P/F ratio is calculated by dividing the pO2 by the FIO2 from the ABG. For example, pO2 is 70 and FIO2 is 0.40. P/F Ratio: 70 / 0.40 = 175. A P/F ratio < 300 indicates acute respiratory failure.Is ARDS the same as acute respiratory failure?
Acute respiratory distress syndrome is a type of respiratory (lung) failure.
How do you assess a patient with respiratory distress?- Check the rate of respiration.
- Look for abnormalities in the shape of the patient’s chest.
- Ask about shortness of breath and watch for signs of labored breathing.
- Check the patient’s pulse and blood pressure.
- Assess oxygen saturation. If it is below 90 percent, the patient likely needs oxygen.
What additional signs would you look for to determine the presence of respiratory distress?
More often, the skin may feel cool or clammy. This may happen when the breathing rate is very fast. Wheezing. A tight, whistling or musical sound heard with each breath can mean that the air passages may be smaller (tighter), making it harder to breathe.
What are three parts of respiratory examination?
- Inspection.
- Palpation.
- Chest percussion.
- Auscultation.
What is AE in respiratory system?
AE is shorthand for Air entry, referring to the intensity of breath sounds. A drawing of lungs with arrows through them, indicates there is nothing abnormal to find on auscultation of the chest.
What are the 4 major functions of the respiratory system?
- Allows you to talk and to smell.
- Warms air to match your body temperature and moisturizes it to the humidity level your body needs.
- Delivers oxygen to the cells in your body.
- Removes waste gases, including carbon dioxide, from the body when you exhale.
What are Covid respiratory symptoms?
People with these symptoms may have COVID-19: Fever or chills. Cough. Shortness of breath or difficulty breathing.
What are 4 types of respiratory infections?
Differences Between the Most Common Respiratory Infections. Four of the most common types of respiratory infections are COVID-19, the flu, pneumococcal disease, and colds.
What are the five most common respiratory infections?
- Upper Respiratory Infections: Common Cold, Sinusitis, Pharyngitis, Epiglottitis and Laryngotracheitis. Etiology: Most upper respiratory infections are of viral etiology. …
- Lower Respiratory Infections: Bronchitis, Bronchiolitis and Pneumonia.
What are the most common early clinical manifestations of ARDS?
The first symptom of ARDS is usually shortness of breath. Other signs and symptoms of ARDS are low blood oxygen, rapid breathing, and clicking, bubbling, or rattling sounds in the lungs when breathing. ARDS can develop at any age.
What is Peep measured in?
This pressure is typically achieved by maintaining a positive pressure flow at the end of exhalation. This pressure is measured in centimeters of water.
Which assessment findings are the earliest indicators of Hypoxemic respiratory failure?
Diagnosis of Acute Hypoxemic Respiratory Failure. Hypoxemia is usually first recognized using pulse oximetry. Patients with low oxygen saturation should have a chest x-ray and ABGs and be treated with supplemental oxygen while awaiting test results.
Is ARDS respiratory acidosis or alkalosis?
In addition to hypoxemia, arterial blood gases often initially show a respiratory alkalosis. However, in ARDS occurring in the context of sepsis, a metabolic acidosis with or without respiratory compensation may be present.
Is ARDS type 1 or type 2 respiratory failure?
Examples of type I respiratory failures are carcinogenic or non-cardiogenic pulmonary edemaa, ARDs, COVID-19 and severe pneumonia. Type 2 – (hypercapnic) respiratory failure has a PaCO2 > 50 mmHg. Hypoxemia is common, and it is due to respiratory pump failure.
What is the difference between respiratory distress and respiratory failure?
Respiratory distress happens when a person is unable to regulate gas exchange, causing them to either take in too little oxygen or expel too little carbon dioxide. Respiratory failure can follow respiratory distress, and causes more severe difficulties with gas exchange. Left untreated, it may be fatal.
What lab values indicate respiratory failure?
One needs to document two of the three criteria to formally diagnose acute respiratory failure: pO2 less than 60 mm Hg (or room air oxygen saturation less than or equal to 90%), pCO2 greater than 50 mm Hg with pH less than 7.35, and signs/symptoms of respiratory distress.
What is the difference between PO2 and PaO2?
PO2 is just partial pressure of oxgen in a given environment, such as room air. … PAO2 is partial pressure of oxygen in alveoli. PaO2 is partial pressure of oxygen dissolved in (arterial) blood.
What does a high pCO2 indicate?
The pCO2 gives an indication of the respiratory component of the blood gas results. A high and low value indicates hypercapnea (hypoventilation) and hypocapnea (hyperventilation), respectively. A high pCO2 is compatible with a respiratory acidosis and a low pCO2 with a respiratory alkalosis.
Which diagnostic tests may be ordered when evaluating a patient with respiratory compromise?
- Radiography.
- Echocardiography.
- Pulmonary Function Tests.
- Right-Sided Heart Catheterization.
Which of the following elements should be checked when assessing respirations?
When measuring and recording respirations the rate, depth and pattern of breathing should be recorded. The depth (volume) of the breath is known as the tidal volume, this should be around 500ml (Blows, 2001). The rate should be regular with equal pause between each breath.
What is chest auscultation?
Chest auscultation involves using a stethoscope to listen to a patient’s respiratory system and interpreting the lungs sounds heard (Physiopedia 2015). Auscultation is a fundamental component of physical examination that can assist in the diagnosis of respiratory issues.
What does Abcde stand for?
The underlying principles are: Use the Airway, Breathing, Circulation, Disability, Exposure (ABCDE) approach to assess and treat the patient.
What is ABC assessment in nursing?
Observing ABCs is a rapid assessment of life-threatening conditions in order of priority. … A is for airway assessment, observing for airway obstruction which can be seen with a changed sound of voice, “see-saw” respirations, and stridor.