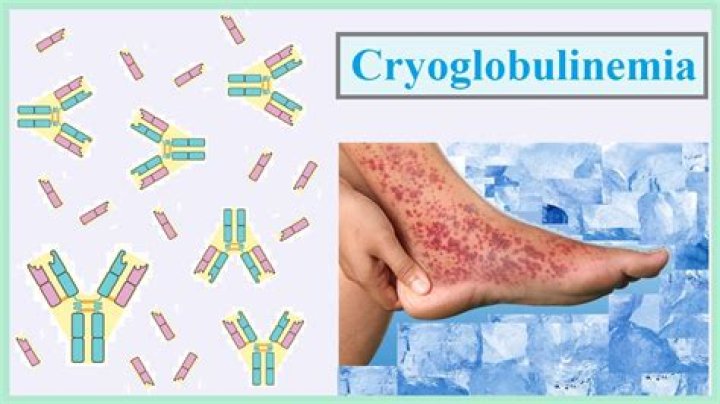
This disorder is due to a cancer of the blood or immune system such as multiple myeloma. Treatment is directed against the abnormal cancer cells that produce the cryoglobulin.
Is cryoglobulinemia serious?
If you have cryoglobulinemia (kry-o-glob-u-lih-NEE-me-uh), these proteins may clump together at temperatures below 98.6 F (37 C). These gelatinous protein clumps can impede your blood circulation, which can damage your skin, joints, nerves and organs — particularly your kidneys and liver.
Is cryoglobulinemia an autoimmune disease?
Mixed cryoglobulinemia is believed to be an immune-mediated disorder (in which the immune system response to chronic infection causes damage to various tissues) or an autoimmune disorder (in which the immune system mistakenly attacks the body’s own tissue).
What is cryoglobulinemia caused from?
Cryoglobulinemia is a disease caused by an abundance of a protein called cryoglobulin in the blood. Cryoglobulins are proteins found in the blood stream that clump together in colder temperatures. These clusters cause blood plasma to become very thick, which can block normal blood flow to tissue and organs.Is cryoglobulinemia a blood disorder?
Cryoglobulinemia is a form of vasculitis—a family of rare disorders characterized by inflammation of the blood vessels, which can restrict blood flow and damage vital organs and tissues.
Can cryoglobulinemia be cured?
The mainstay of treatment is corticosteroids with or without other medications depending on the affected organ and the extent of involvement. Another form of treatment decreases the amount of cryoglobulins in the blood.
Can cryoglobulinemia be fatal?
A potentially life-threatening cryoglobulinemia was considered as the development of renal failure, vasculitic abdominal involvement, pulmonary hemorrhage, or central nervous system involvement. Results: Twenty-nine (14%) patients had life-threatening cryoglobulinemic vasculitis.
What type of doctor treats cryoglobulinemia?
Your treatment team may include specialists in blood (hematologists), connective tissue and arthritis (rheumatologists), liver diseases (hepatologists), the nervous system (neurologists), the kidneys (nephrologists), and other areas as needed.What is essential cryoglobulinemia?
Essential mixed cryoglobulinemia: A condition in which cryoglobulin proteins which are a mixture of various antibody types form for unknown (essential) reasons.
Can cryoglobulinemia cause neuropathy?Cryoglobulinemia is a frequent cause of peripheral neuropathy in undiagnosed referral patients.
Article first time published onHow do you diagnose cryoglobulinemia?
Diagnosis of cryoglobulinemia involves a blood test in which the sample must be kept at normal body temperature, 98.6 F (37 C), for a period of time before being cooled. Inaccurate test results can occur if the blood sample isn’t handled properly.
What does vasculitis pain feel like?
Nerves – inflammation of the nerves can cause tingling (pins and needles), pain and burning sensations or weakness in the arms and legs. Joints – vasculitis can cause joint pain or swelling. Muscles – inflammation here causes muscle aches, and eventually your muscles could become weak.
Why is C4 low in cryoglobulinemia?
Low serum level of complement component 4 (C4) that occurs in mixed cryoglobulinemia (MC) may be due to in vivo or ex vivo activation of complement by the classical pathway.
What causes cryoglobulinemia vasculitis?
The cause of cryoglobulinemic vasculitis is unknown. It occurs mainly in people with a chronic hepatitis C infection. Other viral, bacterial, and fungal infections have also been associated with cryoglobulinemic vasculitis.
What is mixed cryoglobulinemia?
Mixed cryoglobulinemia syndrome (MCS) refers to the presence of either type II or type III cryoglobulins circulating in the serum, which can manifest clinically as a systemic vasculitis with manifestations ranging from purpura, arthralgia, and weakness to more severe neurologic and kidney involvement.
Is vasculitis serious?
Vasculitis can be serious. When your blood vessel becomes weak, it might stretch and bulge (called an aneurysm). It might also burst open, causing bleeding. This can be life-threatening but is very rare.
What is the ICD 10 code for Cryoglobulinemia?
D89. 1 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What blood tests keep you warm?
Cryoglobulin is a common and simple clinical immunology laboratory test that requires the blood samples to be transported to the laboratory, without cooling, at 37°C (1, 5, 6). To achieve this, samples were generally delivered by hand to the laboratory in an insulated container containing warm water.
What causes inflammation of the blood vessels?
Autoimmune disorders, infections, and trauma are some examples of potential triggers of inflammation in the blood vessels. Inflammation in the blood vessels can lead to serious problems, including organ damage and aneurysms. There are many different types of vasculitis.
Does cold weather affect vasculitis?
It usually occurs when the weather is cold and the humidity is high, especially during late fall and winter. It is a form of inflammation of the small blood vessels (vasculitis) that is characterized by painful, itchy, tender, skin injuries (lesions) on the lower legs, hands, toes, feet, ears and face.
What is secondary cryoglobulinemia?
Cryoglobulinemia associated with a particular disease (lymphoproliferative disorder, autoimmune disease, infectious disease) is known as secondary cryoglobulinemia. In a French study of 36 patients with type I cryoglobulinemia, skin or vasomotor symptoms were present in 75%; nephropathy in 30%; and neuropathy in 47%.
What is Cryofibrinogenemia?
Cryofibrinogenemia is a cryoprotein that was first identified in 1955 by Korst and Kratochvil. Unlike cryoglobulin, the precipitate forms only in plasma and not in the serum. The presence of cryofibrinogen in plasma can be asymptomatic.
What is Cryoglobulinemic glomerulonephritis?
Cryoglobulinemic glomerulonephritis (GN) is caused by intracapillary, capillary wall (often subendothelial), and mesangial cryoglobulin deposits, giving a membranoproliferative pattern of injury. Patients have nephritic/nephrotic syndrome with various levels of kidney function.
Does polyarteritis nodosa go away?
There is no cure for polyarteritis nodosa (PAN), but the disease and its symptoms can be managed. The goal of treatment is to prevent disease progression and further organ damage. The exact treatment depends on the severity in each person. While many people do well with treatment, relapses can occur.
What is Cryoglobulin screen?
A cryoglobulins test is used to help detect the presence and relative quantity of cryoglobulins in the blood. It may be ordered along with other tests to help determine or rule out potential causes of cryoglobulinemia. The tests ordered depend on what condition or disease is suspected.
What does vasculitis look like on legs?
Common vasculitis skin lesions are: red or purple dots (petechiae), usually most numerous on the legs. larger spots, about the size of the end of a finger (purpura), some of which look like large bruises. Less common vasculitis lesions are hives, an itchy lumpy rash and painful or tender lumps.
Is vasculitis a terminal illness?
Once considered a fatal disease, vasculitis is now effectively treated as a chronic condition.
What is the life expectancy of someone with vasculitis?
Mean survival time was 126.6 months (95% confidence interval [CI] = 104.5 to 148.6) limited to 154.6 months for the longest-surviving patient.
Does HCV cause cryoglobulinemia?
HCV is a positive strand RNA virus with a 9.6 kb genome that replicates predominantly in the liver. HCV frequently causes extrahepatic manifestations, the most common and severe of which is mixed cryoglobulinemia (MC), a systemic vasculitis affecting small- and medium- sized arteries and veins.
Is Cryoglobulinemia a vasculitis?
Cryoglobulinemic vasculitis (CryoVas) is a small-vessel vasculitis involving mainly the skin, the joints, the peripheral nervous system, and the kidneys. Type I CryoVas is single monoclonal immunoglobulins related to an underlying B-cell lymphoproliferative disorder.
How is polyarteritis diagnosed?
The diagnosis is confirmed by a biopsy showing pathologic changes in medium-sized arteries. The biopsy site may vary. Most biopsies are taken from skin, symptomatic nerve, or muscle. An angiogram of the abdominal blood vessels may also be very helpful in diagnosing PAN.