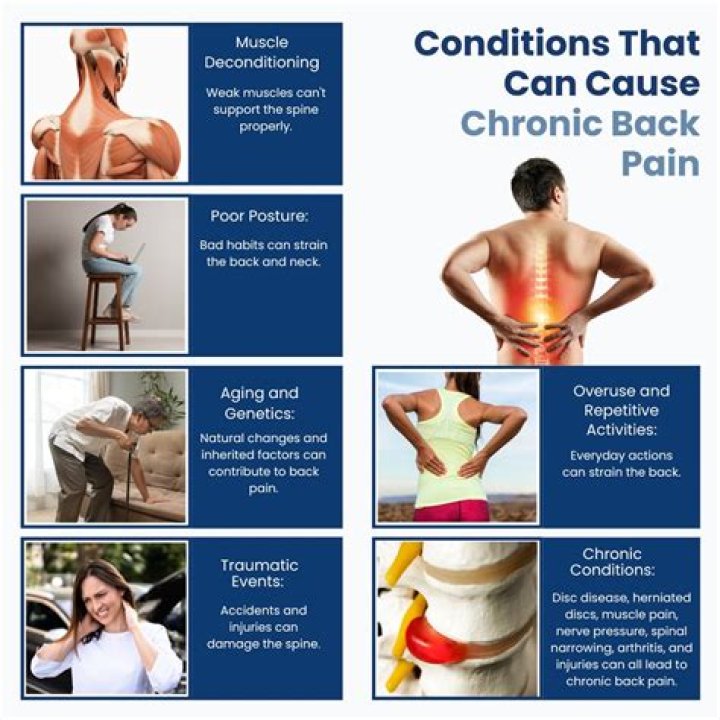
5 – Low Back Pain. ICD-Code M54. 5 is a billable ICD-10 code used for healthcare diagnosis reimbursement of chronic low back pain.
How do you code acute on chronic pain?
In the alphabetical index under PAIN, there is a subheading for “acute” which leads the coder to code R52 Pain, Unspecified. However, listed under R52 is a list of EXCLUDES 1 notes for acute and chronic pain, not elsewhere classified (G89.
What is acute on chronic back pain?
Acute back pain develops suddenly, often as a consequence of an identifiable injury. It can resolve within a matter of days, but may last up to six weeks. Chronic pain tends to develop more gradually over time, and it may become progressively worse.
What is the ICD-10 code for acute on chronic pain?
G89. 29 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.Which is coded first acute or chronic?
If the same condition is described as both acute (subacute) and chronic, and separate subentries exist in the Alphabetic Index at the same indentation level, code both and sequence the acute (subacute) code first.
What is the ICD-10 code for back pain?
ICD-10 code M54. 5, low back pain, effective October 1, 2021.
What is the diagnosis for ICD-10 code r50 9?
9: Fever, unspecified.
What is the ICD-10 code for chronic?
Chronic pain, not elsewhere classified The 2022 edition of ICD-10-CM G89. 2 became effective on October 1, 2021.What is the diagnosis code for acute pain?
ICD-10 code G89. 1 for Acute pain, not elsewhere classified is a medical classification as listed by WHO under the range – Diseases of the nervous system .
What is acute pain?Acute pain begins suddenly and is usually sharp in quality. It serves as a warning of disease or a threat to the body. Acute pain might be caused by many events or circumstances, including: Surgical Pain. Traumatic Pain, example: broken bone, cut, or burn.
Article first time published onWhich is worse acute pain or chronic pain?
Acute pain happens quickly and goes away when there is no cause, but chronic pain lasts longer than six months and can continue when the injury or illness has been treated.
Is a herniated disc chronic or acute?
For example, with a herniated disc, once the pressure on the nerve is alleviated, the acute pain stops. For this reason, medical treatment for acute pain focuses on healing the underlying cause of the pain.
How do you live with chronic lower back pain?
- Learn deep breathing or meditation to help you relax. …
- Reduce stress in your life. …
- Boost chronic pain relief with the natural endorphins from exercise. …
- Cut back on alcohol, which can worsen sleep problems. …
- Join a support group. …
- Don’t smoke.
When should an acute condition be coded?
We go by the rule of thumb that if the provider does not specify acute or chronic we use: Acute: sudden onset and/or has limited duration. Chronic: on-going, usually lasting 6 months or longer.
What are Z codes used for?
Z codes are a special group of codes provided in ICD-10-CM for the reporting of factors influencing health status and contact with health services. Z codes (Z00–Z99) are diagnosis codes used for situations where patients don’t have a known disorder. Z codes represent reasons for encounters.
When do you code chronic conditions?
Chronic conditions must be coded annually with the highest level of specificity. Patients must be evaluated by a medical doctor, a DO, a nurse practitioner, or an advanced practice provider during a face-to-face visit. All chronic conditions should be discussed and documented when meeting with a new patient.
What is the ICD-10 code for CKD?
Chronic kidney disease, unspecified N18. 9 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
What is R53 83?
ICD-10 | Other fatigue (R53. 83)
What is acute febrile illness?
Acute fever or acute febrile illness (a rapid onset of fever and symptoms such as headache, chills or muscle and joint pains) is common in the tropics and sub-tropics and can be caused by very diverse pathogens[1-3].
Is M54 50 a valid diagnosis code?
Code Classification M54. 50 is a billable diagnosis code used to specify a medical diagnosis of low back pain, unspecified. The code M54. 50 is valid during the fiscal year 2022 from October 01, 2021 through September 30, 2022 for the submission of HIPAA-covered transactions.
What is the ICD 10 code for left sided back pain?
2022 ICD-10-CM Diagnosis Code M54. 42: Lumbago with sciatica, left side.
What is back pain M54 9?
ICD-10 code M54. 9 for Dorsalgia, unspecified is a medical classification as listed by WHO under the range – Dorsopathies .
What is diagnosis code z51 11?
11: Encounter for antineoplastic chemotherapy.
What is ICD10 code for fibromyalgia?
ICD-10 Disease codeDescriptionICD M79.0Rheumatism, unspecifiedICD M79.1MyalgiaICD M79.6Pain in limb, hand, foot, fingers and toesICD M79.7Fibromyalgia
What is the CPT code for insomnia?
Insomnia unspecified is classified to code 780.52, and insomnia with sleep apnea goes to code 780.51. Insomnia may be described as primary or secondary. Primary insomnia (307.42) is sleeping problems not directly associated with any other health condition or problem.
When do you use ICD-10 code G89 29?
ICD-10 code G89. 29 for Other chronic pain is a medical classification as listed by WHO under the range – Diseases of the nervous system .
What does ICD-10 code R69 mean?
ICD-10 Code R69: Diagnosis Deferred (Illness, unspecified) has been DELETED from the covered diagnosis list.
Can G89 29 be a primary diagnosis?
ICD-10-CM diagnosis codes do not change. Codes from the “G89” series may be used as the principal diagnosis when the encounter is for pain control or pain management, rather than for management of the underlying conditions.
What is an example of acute pain?
Acute pain typically starts suddenly in response to an injury — a cut, bruise, burn, broken bone, or pulled muscle, for example. Acute pain can also be caused by a fever or infection, labor contractions, and menstrual cramps.
What does acute on chronic mean?
The term acute on chronic is used in medicine to describe situations when someone with a chronic condition, such as chronic obstructive pulmonary disease, also develops an acute condition, such as pneumonia.
What are the difference between acute and chronic?
Acute conditions are severe and sudden in onset. This could describe anything from a broken bone to an asthma attack. A chronic condition, by contrast is a long-developing syndrome, such as osteoporosis or asthma.